By Fabián L. Poletti MD, MSc (DIC), FRCS (Eng), FEBOT (T&O)
Orthopaedic Surgeon and Traumatologist
- A New Perspective on an Ancient Disease
For a long time, osteoarthritis was described as a mechanical consequence of aging: the inevitable “wear and tear” of the joints. It was seen as the price we pay for living and moving.
Today, that view has changed. We now understand that osteoarthritis, particularly knee osteoarthritis, is not merely a problem of “friction” or cartilage erosion. It is a much more complex, multifactorial disease, deeply influenced by the patient’s metabolic, inflammatory, and emotional state.
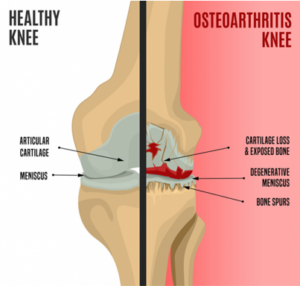
Osteoarthritis is, above all, a chronic low-grade inflammatory disease that develops silently over many years, affecting all the tissues of the synovial joint: cartilage, subchondral bone, synovial membrane, menisci, fat pad, and ligaments.
- Chronic Low-Grade Inflammation: The Invisible Enemy
Acute inflammation is a physiological process: painful, yes, but useful. It is the body’s response to injury. But when inflammation becomes chronic, diffuse, and low-intensity, it ceases to be a defense mechanism and turns into a destructive agent.
This type of inflammation, invisible to the eye and without fever or redness, remains active in the body for years, even decades. And in osteoarthritis, it alters chondrocyte biology, generating a cascade of proinflammatory signals (such as IL-6, TNFα) that weaken tissues and disrupt joint balance.
It’s not a matter of “wear and tear”: it’s a matter of unresolved inflammation.
III. Integrative Medicine: A Complete and Realistic Strategy
Integrative medicine is a way of understanding health that does not oppose conventional medicine but rather broadens and enriches it. It combines scientific knowledge with evidence-based therapies that address the patient holistically: body, mind, and environment.
When we apply this perspective to knee osteoarthritis, the pillars are clear:
- Reduction of systemic inflammation
- Restoration of metabolic and mechanical balance
- Protection and regeneration of joint tissues
- Improvement of functional and emotional quality of life
At the center of all these areas is a fundamental tool: the anti-inflammatory diet.
- Anti-Inflammatory Diet: Treatment Begins in the Kitchen
🔥 Why is diet so important?
Because what we eat directly influences our levels of systemic inflammation. Every meal can act as medicine… or as fuel for the inflammatory fire.
Foods can activate or calm the immune response, modulate gut flora, influence our hormones, and above all, alter the production of cytokines responsible for joint damage in osteoarthritis.

🧠 Key Principles of an Anti-Inflammatory Diet:
💚 1. High in fresh, colorful plant foods
- Fruits and vegetables rich in polyphenols, flavonoids, and carotenoids.
- Especially: berries, purple grapes, broccoli, kale, carrot, spinach, fresh turmeric, ginger, red onion, beetroot, and raw garlic.
💚 2. Healthy but precise fats
- Omega-3: present in fatty fish (wild salmon, mackerel, sardines), chia and flax seeds.
- Extra virgin olive oil, rich in oleocanthal, a compound with anti-inflammatory effect similar to ibuprofen.
- Avoid trans fats and refined oils (sunflower, corn, palm).
💚 3. Quality proteins, in balance
- Prioritize lean proteins: oily fish, organic eggs, white meats.
- Limit red meat to 1–2 times per week.
- Include plant proteins: legumes, quinoa, tofu.
💚 4. Low glycemic index
- Avoid glucose spikes that activate inflammatory pathways.
- Replace white flour with whole grains.
- Limit added sugars, industrial sweets, pastries, and sodas.
💚 5. Key antioxidants and micronutrients
- Vitamin D (eggs, salmon, sun exposure).
- Magnesium (avocado, spinach, almonds).
- Zinc and selenium (nuts, seeds, seafood).
- Curcumin: active when combined with black pepper and healthy fat.
💚 6. Be cautious with ultra-processed foods
- Industrial foods are often loaded with emulsifiers, preservatives, sweeteners, refined oils, and excess salt.
- All of them are linked to an increase in basal inflammatory state.
🍽️ Sample Anti-Inflammatory Day:
Breakfast
Whole grain toast with avocado, tomato, and chia seeds
Green tea or turmeric-ginger infusion
Mid-morning Snack
A handful of walnuts + 1 mandarin
Lunch
Oven-baked salmon with turmeric and lemon
Arugula, beetroot, carrot salad with extra virgin olive oil
Lentils with brown rice (small portion)
Afternoon Snack
Plain yogurt (no sugar) with cinnamon and raspberries
Dinner
Vegetable soup with ginger
Spinach omelet with caramelized onion (no sugar)
Chamomile or lemon balm infusion
🧬 Science Backs It Up
Various studies have shown that a plant-based diet rich in anti-inflammatory compounds and low in ultra-processed foods can:
- Reduce expression of proinflammatory genes like NF-κB.
- Lower IL-6 and TNFα levels in blood and synovial fluid.
- Improve clinical markers like pain, stiffness, and quality of life.
- Enhance the effect of intra-articular treatments like PRP or hyaluronic acid.
- Delay the radiographic progression of the disease.
Recent studies in Mediterranean, Scandinavian, and Asian cohorts confirm that patients with knee osteoarthritis who maintain an anti-inflammatory diet have less need for painkillers and better long-term joint function.
🌿 Phytotherapy and Science-Based Supplements: Natural Allies Against Joint Inflammation
Integrative medicine does not aim to replace necessary medications, but rather to reduce their prolonged use and side effects through natural, science-based resources. Some nutraceutical supplements have demonstrated anti-inflammatory effects comparable to traditional medications, acting on the same biological pathways as NSAIDs, but with a much more favorable safety profile.
Let us look at the most relevant ones:
🟡 Curcumin (Concentrated Extract of Curcuma longa)
Turmeric is a root used for centuries in Ayurvedic medicine. Its most potent active compound is curcumin, a polyphenol with proven anti-inflammatory, antioxidant, and chondroprotective properties.
🔬 Mechanism of Action:
- Inhibits the NF-κB pathway, reducing the transcription of proinflammatory genes.
- Modulates TNFα, IL-6, COX-2, and prostaglandin levels.
- Reduces oxidative stress and improves mitochondrial function.
📚 Scientific Evidence:
- A meta-analysis of 8 clinical trials (Daily et al., 2016) showed that curcumin reduces pain and joint stiffness in knee osteoarthritis comparably to ibuprofen, with better gastric tolerance.
- A double-blind trial (Chandran et al., 2012) compared 500 mg of curcumin twice daily versus 50 mg of diclofenac. The curcumin group had similar pain reduction and notably fewer side effects.
💊 Recommended Dosage:
- 500 to 1000 mg daily of standardized curcumin (with at least 95% curcuminoids).
- Ideally combined with black pepper (piperine) or phospholipids to enhance bioavailability.
🟡 Boswellia serrata (Indian Frankincense)
The resin of the Boswellia tree contains boswellic acids that selectively inhibit the enzyme 5-lipoxygenase (5-LOX), involved in chronic inflammation.
📚 Evidence:
- A randomized study (Kimmatkar et al., 2003) showed that 100 mg of Boswellia extract daily for 8 weeks improved pain and mobility in patients with knee osteoarthritis, with effects comparable to NSAIDs but without their gastrointestinal side effects.
- Another study using AKBA extract (acetyl-11-keto-β-boswellic acid) showed inhibitory effects on cartilage degradation.
💊 Dosage:
- 100 to 250 mg daily of standardized extract, preferably with at least 30% AKBA.
🟡 Omega-3 Fatty Acids (EPA/DHA)
Marine omega-3s have a systemic anti-inflammatory effect by competing with omega-6 fatty acids in the eicosanoid cascade.
📚 Evidence:
- In patients with rheumatoid arthritis, they have been shown to reduce the need for NSAIDs. In osteoarthritis, though the effect is more moderate, they improve morning stiffness and pain in active inflammatory states.
- Reduce markers like CRP, IL-6, and TNFα.
💊 Dosage:
- 1000 to 3000 mg daily of combined EPA + DHA.
- Avoid oxidized supplements or those with poor quality control.
🟡 Ginger Extract (Zingiber officinale)
Like turmeric, ginger acts on cyclooxygenases and lipoxygenases and modulates the inflammatory response at the intestinal, hepatic, and joint levels.
📚 Evidence:
- A double-blind study (Altman et al., 2001) with ginger extract showed significant pain reduction in patients with knee osteoarthritis compared to placebo.
- Other studies compare its effect with ibuprofen, showing similar results after 3 months with better gastrointestinal tolerance.
💊 Dosage:
- 500 to 1000 mg daily of concentrated extract (not raw powder).
- Can be combined with turmeric for a synergistic effect.
🟡 UC-II (Undenatured Type II Collagen)
Unlike hydrolyzed collagen, native type II collagen acts via oral immunomodulation, promoting oral tolerance to joint antigens.
📚 Evidence:
- Clinical trials show that 40 mg daily of UC-II improves function and reduces pain in knee osteoarthritis, with effects similar or superior to glucosamine.
- It has chondroprotective and anti-inflammatory action.
🟡 Useful Clinical Combinations
Many effective supplements combine:
- Curcumin + Boswellia + Ginger
- UC-II + Hyaluronic Acid + Vitamin C
- Omega-3 + Vitamin D + Polyphenols (Resveratrol, Quercetin)
These combinations are designed to act on multiple levels of inflammation, with positive synergy and without the adverse effects of NSAIDs.
⚠️ Important: Individualize and Advise
Although these supplements have scientific backing, they should not be taken without medical supervision, especially in patients with:
- Liver or kidney disease
- Use of anticoagulants
- Interactions with immunosuppressive drugs
A personalized assessment and progressive approach are key to incorporating these resources safely and effectively.
🧘♂️ What Else is Part of the Integrative Approach?
Diet is only one pillar. The integrative approach is completed with:
- Adapted and regular physical exercise
- Body weight control
- Regenerative interventions (PRP, hyaluronic acid)
- Chronic stress management (mindfulness, breathing, psychological therapy)
- Restorative sleep
- Evidence-supported complementary therapies (acupuncture, thermotherapy, fascial massage)
🌟 Conclusion: Transform, Support, and Heal Through a Wiser Lens
Knee osteoarthritis has no definitive cure. But that doesn’t mean there is no hope. On the contrary: we can prevent its progression, relieve symptoms, improve joint function, and above all, change the narrative with which patients face their diagnosis.
Taking care of what we eat is taking care of our joints. But it’s not just about food: how we move, how we rest, how we manage stress, and how much space we give to our overall health also matter. Integrative medicine offers a broad, human, and scientifically grounded strategy that allows us to approach this disease from all angles.
When surgery is not yet necessary — and often we can delay that moment — there are safe and effective options that complement the integrative treatment. Intra-articular injections of hyaluronic acid, platelet-rich plasma (PRP) or other regenerative therapies, when properly indicated, can help reduce pain, improve mobility, and slow joint degeneration.
Osteoarthritis cannot be treated with simplistic solutions. It requires science, sensitivity, and long-term vision. It requires listening to the patient, walking beside them, and offering real, personalized, and sustainable tools.
As an orthopaedic surgeon and researcher, but also as a physician who listens, explains, and supports, I am deeply convinced that well-applied integrative medicine is one of the best tools of the 21st century for treating complex chronic diseases like osteoarthritis. We may not always be able to cure. But we can transform. And that, in medicine, is often the most valuable gift we can offer.
Leave a Reply