Patellar Maltracking and Instability
What is Patellar Maltracking and Instability?
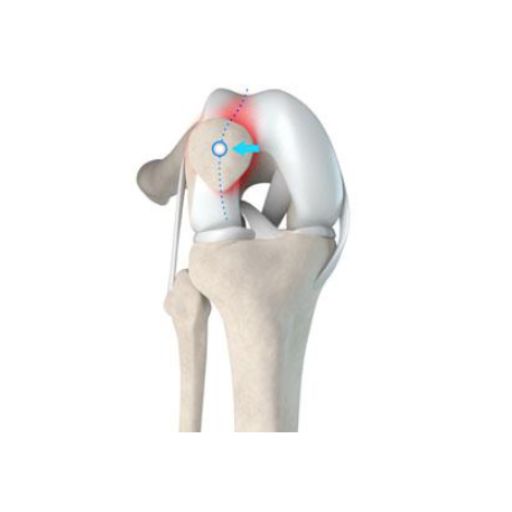
Patellar instability occurs when the kneecap (patella) repeatedly dislocates or partially dislocates (subluxates) from its natural position in the femoral groove—the track in which it glides during knee movement. The patella plays a critical role in knee biomechanics, facilitating smooth motion and force distribution. It is stabilized by ligaments and muscles, which keep it properly aligned. However, when these stabilizing structures are weakened or damaged, the patella may: 🔹 Partially slip out of place (subluxation) 🔹 Completely dislocate from the femoral groove Recurrent patellar maltracking can further damage the ligaments, cartilage, and muscles that support the knee, worsening instability and pain over time.
Symptoms of Patellar Maltracking and Instability
Patients with patellar instability often experience: ✔ Pain – Especially when transitioning from sitting to standing, squatting, or walking upstairs. ✔ A sensation of knee instability – A feeling that the knee may "give way" or buckle. ✔ Recurrent patellar subluxations or dislocations – Increasing with activity. ✔ Visible deformity – The kneecap may appear out of place following a dislocation. ✔ Swelling and stiffness – Resulting from irritation of soft tissues. ✔ Reduced knee function – Difficulty engaging in activities like sports, running, or even walking long distances. Early diagnosis and appropriate treatment are essential to prevent further joint damage and restore knee function.
Causes and Risk Factors for Patellar Maltracking and Instability
Several anatomical and biomechanical factors contribute to patellar instability: 🔹 Anatomical Abnormalities Congenital variations in patellar shape or femoral groove anatomy. Flat feet (pes planus) – Can alter lower limb alignment, increasing instability. 🔹 Abnormal "Q" Angle The Q angle represents the angle between the hip and knee. A higher Q angle, commonly found in patients with knock knees (genu valgum), increases lateral forces on the patella, predisposing it to maltracking. 🔹 Muscular Imbalances The quadriceps, particularly the vastus medialis obliquus (VMO), plays a crucial role in keeping the patella centered in the groove. Weak or imbalanced thigh muscles can allow the patella to drift laterally, leading to instability. 🔹 Ligamentous Laxity or Injury The medial patellofemoral ligament (MPFL) prevents excessive lateral movement of the patella. If this ligament is torn or stretched, even minor movements can trigger a dislocation. 🔹 Rotational and Coronal Deformities In some cases, bony alignment abnormalities in the femur or tibia contribute to patellar instability, including: ✔ Femoral Anteversion – Excessive inward rotation of the femur, leading to malalignment of the knee and patella. ✔ External Tibial Torsion – Outward twisting of the tibia, affecting the mechanics of the knee joint. ✔ Coronal Plane Deformities – Most commonly valgus (knock-knee) alignment, which increases the lateral pull on the patella. In such cases, rotational osteotomies (femoral or tibial) or coronal osteotomies may be necessary to correct these misalignments and restore knee stability.
Diagnosing Patellar Maltracking and Instability
A comprehensive diagnostic approach is necessary to assess knee alignment, stability, and soft tissue integrity. The evaluation typically includes: ✔ Clinical Examination – Assessing patellar tracking, ligament stability, and muscle balance. ✔ X-Rays – Evaluating patellar position, bone alignment, and potential deformities. ✔ MRI (Magnetic Resonance Imaging) – Examining the MPFL, cartilage, and soft tissue structures. ✔ CT Scan (if needed) – Providing detailed 3D imaging to assess rotational deformities or trochlear dysplasia. A precise diagnosis guides treatment planning, ensuring the best surgical or non-surgical intervention.
Treatment Options for Patellar Maltracking and Instability
The treatment strategy depends on the severity of instability, the underlying cause, and the patient’s functional goals. 🔹 Non-Surgical (Conservative) Management For mild cases, initial treatment focuses on improving muscle strength, alignment, and stability through: ✔ Physical Therapy – Strengthening the quadriceps and VMO to enhance patellar tracking. ✔ Bracing & Orthotics – Knee braces and foot orthotics to support proper alignment. ✔ Pain Management – Anti-inflammatory medications or PRP (Platelet-Rich Plasma) injections to reduce swelling and discomfort. ✔ Activity Modification – Avoiding high-impact activities until knee stability improves. However, if patellar instability is recurrent or associated with significant anatomical abnormalities, surgical intervention may be required. 🔹 Surgical Treatment for Patellar Instability Surgery aims to restore patellar alignment and correct structural abnormalities. The most commonly performed procedures include: 🔹 MPFL Reconstruction (Medial Patellofemoral Ligament Reconstruction) Restores the primary ligament preventing lateral dislocation. Uses a tendon graft to replace the damaged MPFL and improve stability. 🔹 Tibial Tubercle Osteotomy (Tibial Tubercle Transposition – TTT) Repositions the patellar tendon attachment to improve tracking. Helps redirect the pull of the quadriceps, reducing lateral displacement. 🔹 Trochleoplasty Performed in patients with trochlear dysplasia (a shallow or absent femoral groove). Reshapes the trochlea, creating a deeper track for the patella to stay in place. 🔹 Rotational Osteotomies (Femoral or Tibial) Necessary when femoral anteversion or tibial torsion contribute to maltracking. Femoral osteotomy corrects excessive internal rotation of the femur. Tibial osteotomy addresses external rotation or coronal deformities (e.g., valgus knee). These procedures correct the mechanical alignment of the lower limb, ensuring proper patellar function.
Post-Surgical Recovery & Rehabilitation
Recovery is structured and progressive, focusing on: ✔ Phase 1 (0-6 weeks) – Initial healing, limited weight-bearing, controlled range-of-motion exercises. ✔ Phase 2 (6-12 weeks) – Quadriceps strengthening, balance training, and gait correction. ✔ Phase 3 (3-6 months) – Sport-specific drills, dynamic knee stability exercises, and full return to activity. A well-structured rehabilitation program is key to long-term success.
Why Choose Dr. Fabián Poletti for Patellar Instability Treatment?
As an internationally trained Consultant Orthopaedic and Trauma Surgeon, Dr. Fabián Poletti specializes in advanced knee surgery and complex patellar instability cases. His approach integrates: ✔ Minimally invasive techniques for reduced recovery time. ✔ Personalized surgical planning, considering individual knee biomechanics. ✔ State-of-the-art procedures, including MPFL reconstruction, trochleoplasty, tibial tubercle osteotomy, and rotational osteotomies. ✔ Enhanced rehabilitation protocols for rapid return to normal activities and sports. With training in Florence, London, Oxford, and Madrid, Dr. Poletti ensures precision, innovation, and excellent patient outcomes. 📩 Book a Consultation If you experience persistent knee instability, recurrent dislocations, or pain affecting your mobility, seeking specialist care is crucial to restore function and prevent further damage. 📍 Location: Hospiten Estepona, Costa del Sol 📩 Contact: Schedule an appointment via website or social media. 🔹 Stabilize your knee. Move with confidence. 💪🏼🚀