Total Knee Replacement (Total Knee Arthroplasty)
(for russian and italian, scroll down)
What is a Total Knee Replacement?
Total knee replacement (TKR), also known as total knee arthroplasty, is a surgical procedure designed to restore function, reduce pain, and improve quality of life in patients suffering from severe knee arthritis or joint damage. This involves removing the worn-out or damaged surfaces of the knee joint and replacing them with biocompatible metal and plastic implants, replicating the natural movement of a healthy knee.
A well-performed knee replacement not only alleviates pain but also enhances mobility, allowing patients to return to daily activities, sports, and an active lifestyle.
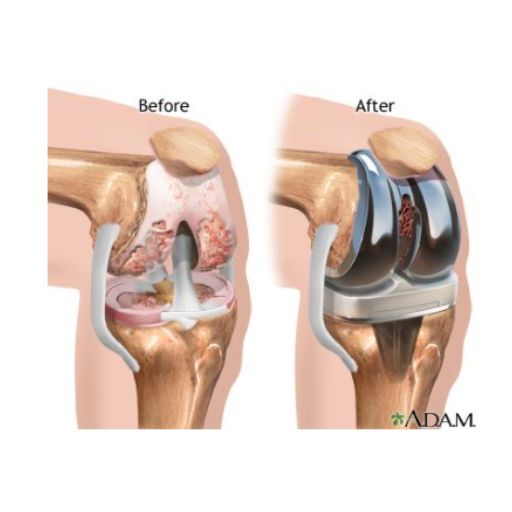
Understanding Knee Arthritis
The knee is a complex biomechanical structure, composed of: Femur (thighbone) Tibia (shinbone) Patella (kneecap)
Each of these bones is covered by articular cartilage, a smooth, shock-absorbing layer that facilitates frictionless movement. Additionally, the menisci—two C-shaped cartilaginous structures—act as cushions, distributing weight and reducing stress on the joint. Over time, due to aging, mechanical wear, trauma, or degenerative diseases, the articular cartilage deteriorates, leading to bone-on-bone contact. This process, known as arthritis, results in pain, stiffness, swelling, and limited mobility. One of the most common forms of arthritis affecting the knee is osteoarthritis, a degenerative condition that gradually erodes the joint surfaces, often leading to the formation of bone spurs (osteophytes), further restricting movement and causing discomfort.
Causes of Knee Osteoarthritis
While the exact cause of osteoarthritis remains multifactorial, several key risk factors contribute to its development: ✔ Previous knee trauma or fractures ✔ Obesity or excess weight (increased joint load) ✔ Repetitive stress or overuse (e.g., high-impact sports, heavy labor) ✔ Inflammatory joint conditions (e.g., rheumatoid arthritis) ✔ Congenital or genetic factors affecting joint alignment ✔ History of joint infections
Diagnosing Knee Osteoarthritis
A comprehensive evaluation is essential for an accurate diagnosis and tailored treatment plan. This typically includes: 🔹 Detailed medical history & physical examination 🔹 X-rays to assess joint space narrowing, bone spurs, and deformities 🔹 MRI (if needed) to evaluate cartilage integrity, meniscus damage, or soft tissue injuries Once a diagnosis is established, treatment recommendations are made based on the severity of joint deterioration and impact on daily life.
When is a Total Knee Replacement Recommended?
Total knee replacement is indicated when: ✅ Severe knee pain affects daily activities such as walking, standing, or climbing stairs. ✅ Persistent pain at rest, especially at night, disrupting sleep. ✅ Chronic swelling and inflammation unresponsive to medication or conservative therapies. ✅ Failure of non-surgical treatments, including weight loss, physiotherapy, medications, and intra-articular injections (PRP, hyaluronic acid). ✅ Significant knee deformity (bow-legged or knock-kneed alignment). If at least two of the three knee compartments (medial, lateral, and patellofemoral) are affected, a total knee replacement is the best surgical option.
The Total Knee Replacement Procedure
Surgical Goals
✔ Pain relief ✔ Restoration of joint alignment & mobility ✔ Long-term functionality & implant durability
Total knee replacement is performed under spinal or general anesthesia. The steps include:
1️⃣ Incision & Joint Exposure The surgeon makes an incision over the knee to carefully access the joint. 2️⃣ Removal of Damaged Bone & Cartilage The damaged femur (thighbone) and tibia (shinbone) surfaces are precisely reshaped. Specialized surgical guides (jigs) ensure optimal bone resection and alignment. 3️⃣ Implant Placement A metal femoral component is securely attached to the femur using biocompatible bone cement. A tibial component is fixed onto the reshaped tibia. A highly durable polyethylene insert is placed between these components to ensure smooth, frictionless movement. 4️⃣ Patella Preparation The undersurface of the kneecap is modified, and a patellar implant may be added to optimize tracking over the new knee joint. 5️⃣ Final Testing & Closure The joint is carefully tested through full range of motion to confirm stability and proper function. The incision is meticulously closed, and a sterile dressing is applied. Total surgery time: 1-2 hours.
Recovery & Postoperative Care
Early mobilization is essential for a successful outcome. The enhanced recovery protocol includes: ✔ Walking within hours of surgery with crutches or a walker. ✔ Physical therapy starts immediately, focusing on strengthening, balance, and joint mobility. ✔ Personalized rehabilitation plan to restore function and independence. ✔ Full recovery timeline: Initial functional recovery: 2-6 weeks Return to daily activities: 6-12 weeks Full recovery & sports activities: 3-6 months
⚠️ Risks & Potential Complications
While knee replacement is a highly successful procedure, as with any major surgery, some risks include: 🔹 Infection 🔹 Blood clots (deep vein thrombosis, pulmonary embolism) 🔹 Nerve or blood vessel injury 🔹 Implant loosening or wear over time 🔹 Persistent knee stiffness or limited motion Fortunately, with modern surgical techniques, meticulous implant selection, and a well-planned recovery program, these risks are minimized.
Why Choose Dr. Fabián Poletti for Your Knee Replacement?
Dr. Fabián Poletti is an internationally recognized Consultant Orthopaedic and Trauma Surgeon, specializing in knee surgery and joint reconstruction. His approach to total knee replacement integrates: ✔ Patient-specific implant selection tailored to individual anatomy. ✔ Minimally invasive techniques to preserve soft tissues and enhance recovery. ✔ Advanced alignment methods (kinematic alignment, medial pivot implants). ✔ Technology-assisted surgery (computer navigation, augmented reality). ✔ Enhanced recovery protocols – walk within 2 hours, discharge within 24-36 hours.